#News
#News
Historical threats
Researchers seek to understand diseases that affect Indigenous populations
 Crédito: Rômolo D’Hipólito / Estúdio Voador
Crédito: Rômolo D’Hipólito / Estúdio Voador
The Javari Valley, at the western end of the state of Amazonas, became the subject of global
news in 2022 with the deaths of Indigenous expert Bruno Pereira and journalist Dom
Phillips, murdered for investigating environmental crimes in the region. Accounts of the
dramatic situation made an impression on nurse Eliseth Ribeiro Leão, a researcher at Hospital
Israelita Albert Einstein (HIAE), in part because she had visited the area in person, but under
very different circumstances.
A decade ago, Leão and her then master’s advisor, Elaine Barbosa de Moraes, visited the
region for a pioneering study on how the Javari Valley’s different Indigenous groups dealt with
bodily pain and headaches. “We traveled through all the places linked to the Dom and Bruno
case. At times, when discussing this, we would even ask ourselves ‘Wow, were we actually
there?’ Because that’s how we feel. It seems like another place, another country,” she says.
This chasm between the rest of Brazil and many of the Indigenous populations in the Amazon
region and other areas is also reflected in health conditions. The HIAE researchers’ work, which
also included visiting Indigenous communities in Acre, has shown that the prevalence of lower
back pain is nearly three times higher among Indigenous people of the Amazon than the
Brazilian population as a whole, while that of headaches is nearly double. Recent surveys
indicate that a similar picture applies not only to pain, but also to other health indicators,
reflecting problems that affect Indigenous groups worldwide.
Ricardo Ventura Santos, of the Oswaldo Cruz Foundation’s National School of Public Health
(FIOCRUZ), recalls that a study published in The Lancet in 2016, conducted by Ian Anderson, of
the University of Melbourne, in Australia, provided a broad overview of the problem at a
global level. “It’s a study in which we also participated, which compares the health indicators
of Indigenous peoples and the benchmark population, namely the national non-Indigenous
populations from each place,” he explains.
During this study, which gathered information on 28 Indigenous communities from 23
different countries, Anderson and his colleagues identified systemic differences—favoring non-
Indigenous populations over Indigenous groups—in matters such as life expectancy at birth,
infant and maternal mortality, child malnutrition, and childhood and adult obesity. “I think that
it is the most important and comprehensive study of the last decade on this subject,” says the
FIOCRUZ researcher.
Markers of colonialism
Factors that explain this disparity, regarding the public health issues experienced by Brazilian
Indigenous communities, are complex and varied, but all are linked, to some extent, to the
history of colonialism and to the social exclusion that has affected these people since the
Europeans’ arrival—and which has intensified over the last century, particularly for Amazonian
communities.
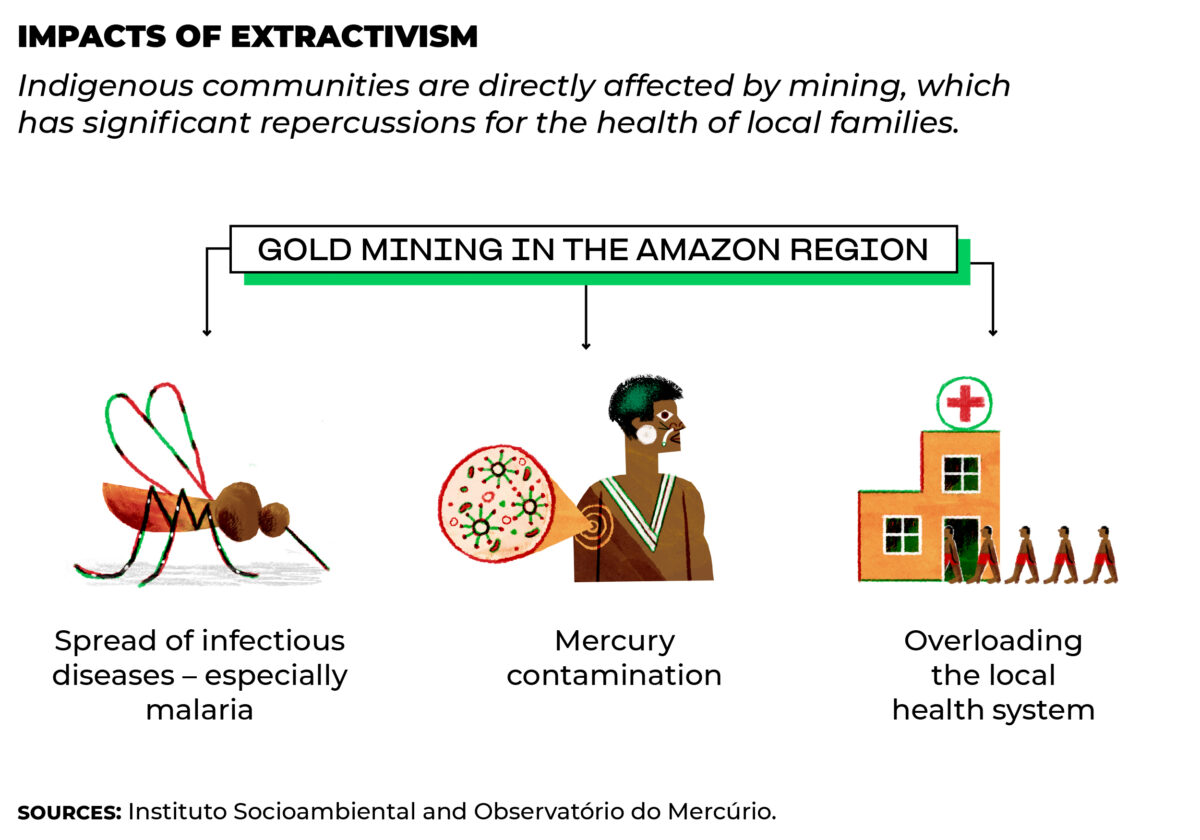
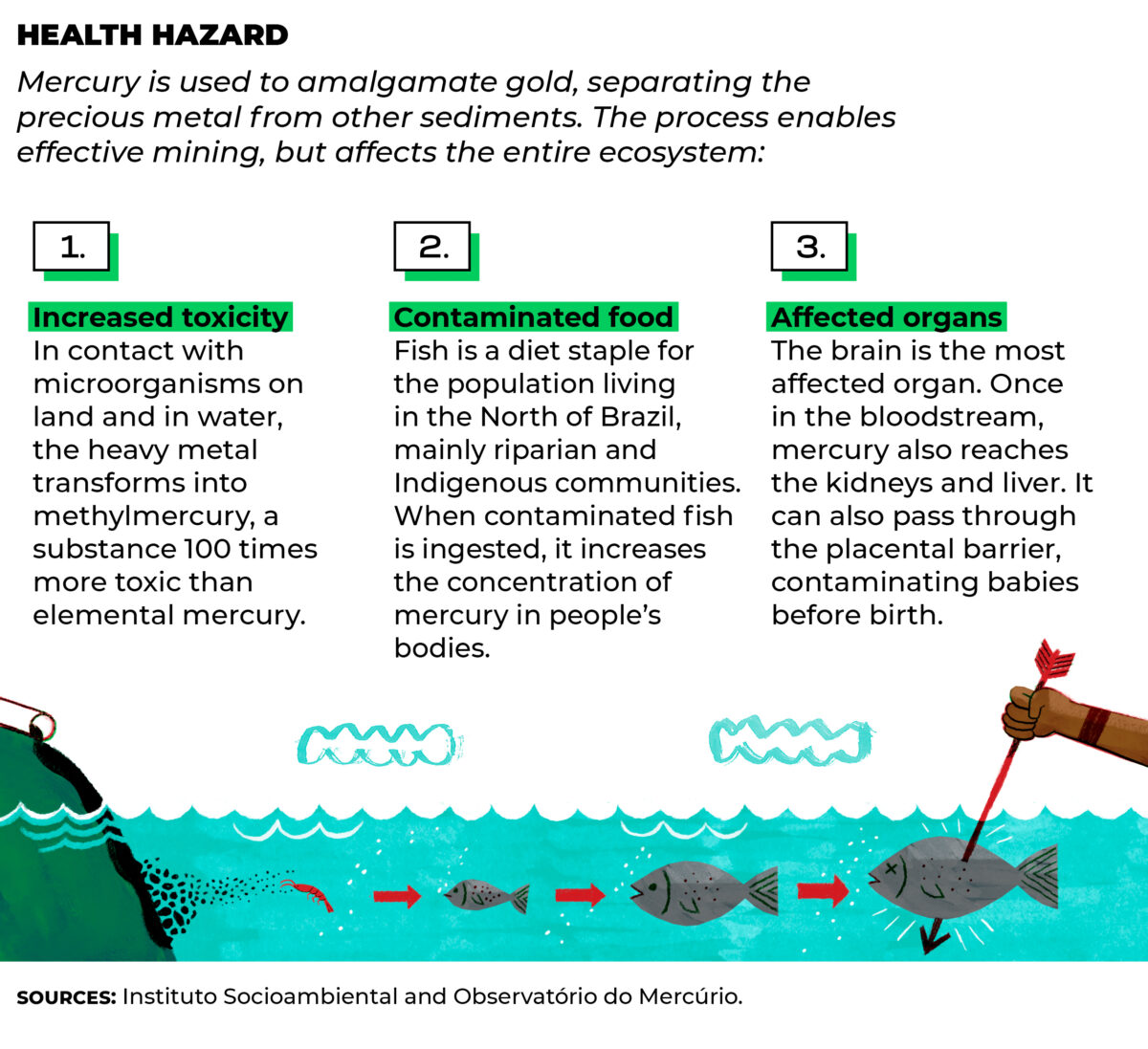
For starters, the systemic loss of traditional territories to loggers and ranchers and the
contamination of rivers by mining operations have significantly impacted the livelihoods of
these populations, jeopardizing their food security and, therefore, their health.

Additionally, similar to other Indigenous groups in the Americas, the Brazilian Indigenous communities did not initially have any type of immunity against Old World infectious diseases, particularly zoonotic diseases transmitted by pets never before bred on this side of the Atlantic.
Health problems in Indigenous communities are complex and varied, but all are linked to the history of colonialism and social exclusion
Many deaths have been caused by these diseases since first contact with the Portuguese.
Estimates made by archaeologists such as Eduardo Góes Neves, of the Museum of Archaeology
and Ethnology at the University of São Paulo (MAE-USP), indicate that the Amazon region’s
population before the European invasion may have reached 10 million inhabitants, most of
which likely perished as a result of infectious diseases in the first centuries following 1500.
However, this process still occurred quite frequently between 1960 and 1970, when the
military dictatorship’s initiatives aimed at economic exploitation and geopolitical occupation of
the Amazon region resulted in lethal outbreaks of diseases such as measles and the flu among
newly contacted groups. The continued presence of isolated communities in the region to this
day means that the possibility of this occurring is not completely out of the question.
Furthermore, in recent decades, even ethnic groups with a relatively brief history of contact
with non-Indigenous society are going through what can be classified as a nutrition transition.
Economic transformations in the areas surrounding Indigenous land, including more
streamlined transportation and communication, and the integration of these group members
into the labor market and welfare programs, may encourage the incorporation of processed
products into their diets. This tends to increase the consumption of cheap foods that are rich
in carbohydrates and low in nutritional value (pasta, soda, etc.), which has led to a higher rate
of cardiovascular diseases, obesity, and diabetes.
Genetic research
In recent decades, some studies have sought to investigate whether Indigenous populations’ vulnerability to these problems is linked to a genetic component, considering their evolutionary isolation from their ancestors in the Americas during the last 15,000 years. Currently, there is little evidence of this. “It is important to highlight that these populations are very neglected and that we still have few answers about Indigenous genetics and health,” considers Tábita Hünemeier, a researcher at the University of São Paulo’s Institute of Biosciences (IB-USP).
According to her, in the case of diseases that have become more common thanks to the consumption of processed foods, there are already some studies pointing to the presence of genetic variants that would favor this type of ailment. Among them is a version of the ABCA1 gene, linked to cholesterol metabolism, which is the topic of a 2011 study coauthored by Hünemeier. “It is the only one that shows a variant exclusive to Indigenous peoples of the Americas that leads to such phenotypes, but there are others that show a higher frequency of variants that favor such diseases in Indigenous peoples,” she explains.
Maria Cátira Bortolini, a geneticist at the Federal University of Rio Grande do Sul (UFRGS) and coauthor of the ABCA1 study, says that her group is seeking to involve Indigenous students at the university in related projects. “A Kaingang student majoring in dentistry should work with us on a project about oral metagenomics [that is, the genomes of populations of organisms in the mouth],” she says. “This is very exciting.”
Considering that other groups around the world also have their own genetic vulnerabilities in relation to caloric food, Ventura Santos says that this data must be handled prudently. “Often, this ends up attracting more attention than models of the social determinants of the disease process,” he considers.
In a study recently published by the researcher and other FIOCRUZ colleagues in the Oxford Research Encyclopedias of Global Public Health, the impact of these determinants is quite clear, as is the fact that there have been significant improvements in the Indigenous public health system in recent decades, despite major problems that persist.
The consumption of cheap foods that are rich in carbohydrates and low in nutritional value has led to a higher rate of cardiovascular diseases, obesity, and diabetes
A case that helps illustrate this is that of the Suruí-Paiter of Rondônia, studied by the FIOCRUZ
researchers since the 1980s. Data from 1987 showed that nearly half of Suruí children up to
nine years of age demonstrated stunted growth, an indicator linked to a number of other child
development variables.
In 2005, however, the proportion of boys and girls in this community with stunted growth
dropped to a quarter of the previous total, while childhood obesity began to be detected in
this population (in 3.9% of children). “These findings were important motivators to drafting a
nutritional policy for Indigenous peoples in Brazil, and for showing that Indigenous children do
not ‘naturally’ have short stature, as many believe,” wrote the authors. They also highlight
advances in vaccination campaigns and decreasing child mortality, in part due to the 1999
creation of the Indigenous Health Subsystem within the Brazilian Unified Health System (SUS).
Bodily pain
According to the study conducted by Einstein Hospital researchers on pain, published in 2021 in the Journal of Pain Research, the impact of medical assistance is coupled with traditional strategies to relieve pain. Among the 90 study participants, belonging to the Matis, Marubo, Kanamary, Ashaninka, and Huni Kuin communities, both non-Indigenous medicine and the traditional medicine from each culture were used by about 70% of people. “We see frequent use of traditional, topical preparations,” describes Eliseth Leão.
According to the researcher, the constant physical effort dictated by the lifestyle in Indigenous communities helps explain the high prevalence of bodily pain, well above the Brazilian average. “I remember seeing an elderly man, squatting down and digging dirt with his bare hands, filling an aluminum bucket with the dirt, tossing the bucket, and coming back to dig more,” she says.
“Women also carried heavy things, from clothes to wash in the river to children. One time, I even mentioned this to one of them and she responded, laughing: ‘Wow, you’re really weak, aren’t you?’ So it seems there is a certain stoicism there, a threshold for coping with pain that is mediated by culture,” analyzes the researcher.
According to Leão, the plan is to carry out a third expedition, expanding the range of communities studied. Project funding, provided by an Einstein Hospital donor, is even allocated to this, but the COVID 19 pandemic hindered the team’s plans. The disease heavily affected the Brazilian Indigenous communities, which needed to legally mobilize in order to be included in the priority groups for vaccination.
“People know very little about the situation—we live as if they didn’t exist. Anyone in a place that prioritizes knowledge generation, like Hospital Israelita Albert Einstein, is responsible for shedding some light on all of this,” she says.
*
This article may be republished online under the CC-BY-NC-ND Creative Commons license.
The text must not be edited and the author(s) and source (Science Arena) must be credited.