 #Columns
#Columns
Polio is not gone: how to be ready
As long as the virus still exists in some corner of the world, it is just a plane ride away from us
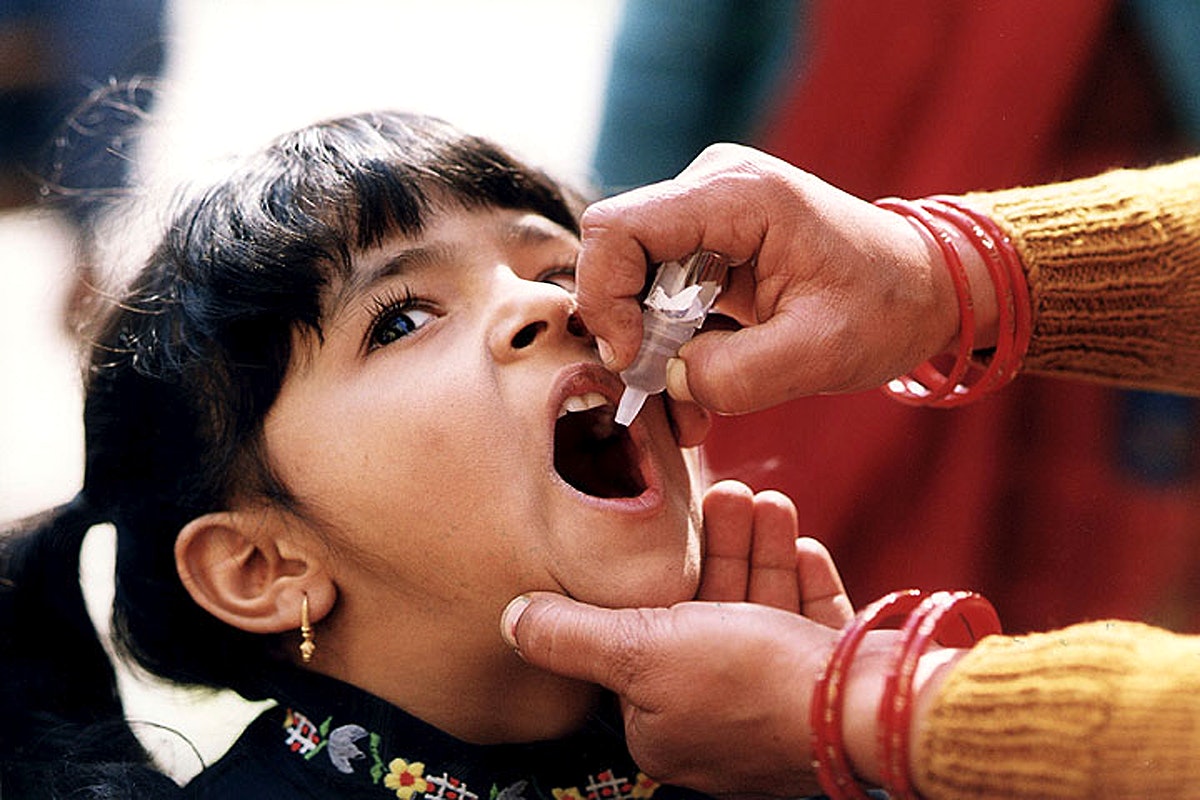 Centers for Disease Control and Prevention/US Gov
Centers for Disease Control and Prevention/US Gov
In the early 20th century, polio was one of the most feared diseases, paralysing hundreds of thousands of children every year. Polio cases peaked in 1988 at 350.000 cases despite the long availability of two vaccines – the Salk inactivated polio vaccine IPV and the Sabin life attenuated polio vaccine OPV. These two vaccines are very different: the Sabin OPV provides besides humoral also intestinal immunity. In very rare circumstances the OPV vaccine virus would revert to virulence causing vaccine-associated paralytic polio in the vaccines (VAPP). In populations with low immunisation coverage OPV which is shed in stool circulates in the community and might loose its attenuating mutations.
These “circulating vaccine-derived polioviruses (cVDPVs)” can behave like wild-type polioviruses and might cause outbreaks. The inactivated Salk IPV is not associated with this risk but also does not induce intestinal or herd immunity. Polio can be eradicated – humans are the only natural host and efficient vaccines are available. This goal was missed. Thus the World Health Assembly established in 1988 the Global Polio Eradication Initiative GPEI mandating polio eradication by 2000. This goal was missed. WHO declared wild-type poliovirus type 2 eradicated in 2015 and initiated by a globally coordinated stop of all routine use of serotype 2 containing oral polio vaccines (OPV2).
In 2019 also wild-type poliovirus type 3 was declared eradicated. Thus, polioviruses 2 and 3 are the only other two viruses eradicated from earth besides smallpox. Poliovirus type 1 continues circulating endemically in small geographical pockets in Pakistan and Afghanistan but virus exportation occurred with clinical cases of PV1 earlier this year in Malawi and Mozambique, countries which were polio free since long.
The switch from trivalent OPV to IPV/ bivalent type 1 and 3 OPV and the global cessation of use of OPV2 in 2016 did however not end circulation of vaccine derived type 2 polio cVDPV2. Cases and outbreaks of cVDPV2 jumped in various countries because of insufficient vaccination coverage and low population immunity to prevent VDPV circulation prior to the switch, from 71 cases in 2018 to 531 within the last 12 months. 499 of those which were cVDPV2. In contrast, there were just 33 cases of wild-type 1 polio reported during the same period.
Surveillance for acute flaccid paralysis is an important tool to identify polio but case detection might come late. A recent study from Israel showed that after importation of a wild-type PV1 over 7,000 people became infected without a single paralytic case. To supplement AFP surveillance sewage sampling is the best method for early detection of PV circulation, often much before symptomatic cases appear.
Tools to contain a cVDPV2 outbreak are limited: IPV does not induce sufficient intestinal immunity to stop viral circulation. Sabin mOPV2 induces herd immunity but is also causing VDPV2 outbreaks as it is genetical instable and can revert to virulence: fighting fire with fire. A scientific consortium supported by BMGF was tasked to develop a genetically more stable novel OPV2 (nOPV2) that would maintain the advantages of Sabin OPV2 but with a reduced risk of reversion to virulence.
BMGF also supported a group of worldwide experts, which I am part of, to design an emergency clinical development program that started in 2018. The studies – most of them performed in Latin America – showed that nOPV2 was as safe and as immunogenic as Sabin OPV2 but much more genetically stable. Since WHO Emergency Use Listing (EUL) in 2020 over 500 million doses of nOPV2 have been distributed. So far there is no evidence for breakthrough transmission nor an emergence of cVDPV’s related to nOPV2.
What is the relevance for Brazil and other Latin American countries? Importation of wild-type PV and occurrence of VDPV outbreaks might appear to be a problem for resource limited countries in specific geographies. But recent incidents show that Polio is an international concern: wild type PV1 was imported to Israel and detected in sewage in various sampling locations; VDPV2 was detected in multiple wastewater samples in London; an acute flaccid paralysis in an unvaccinated US citizen was caused by cVDPV2, indicating that there was likely substantial polio virus circulation in this community despite that the US stopped the use of oral polio vaccines decades ago.
In Brazil an AFP is under investigation. Polio remains a global threat, and PAHO has warned that countries are at high risk for reintroduction of polio, following a drop in vaccination rates.
To be prepared, strong surveillance of AFP; wastewater surveillance and sequencing of isolated viruses to determine extent and origin of any contamination should be strengthened. Ensure high priming coverage with IPV, booster and catch-up immunisation programs prioritising unvaccinated individuals should be an immediate first step to ensure individual protection. nOPV2 is the vaccine of choice for outbreak control – to ensure availability “just in case” an EUL by the national regulatory authority should be obtained now and access to stockpiles should be secured.
Polio is not gone. As long as the virus still exists in some corner of the world, it is just a plane ride away from us.

Sue Ann Costa Clemens is Head of the Institute for Global Health at the University of Siena, where she is Director of the Masters Program in Vaccinology and Drug Development and Professor of Pediatric Infectious Diseases. She is a Global Health and Clinical Development Professor at the University of Oxford, Director of the Oxford Latam Vaccines Group, and Professor and International Scientific Coordinator at the Carlos Chagas Institute. She has been a Senior Advisor to the Bill and Melinda Gates Foundation since 2012 and is a member of scientific advisory boards at several institutions. In 2023, she was a World Health Organization Expert Group on Access and Information on Vaccines (TAG-MI4A) member. She has contributed to developing more than 20 globally licensed vaccines and medicines over a career spanning more than 25 years. Sue Ann was awarded the Order of the British Empire, CBE, by Queen Elizabeth II for services to Public Health; she is also a Commander of the Federative Republic of Brazil in the Orders of Rio Branco and Medical Merit.
Opinion articles do not necessarily reflect the views of Science Arena or Hospital Israelita Albert Einstein.
*
This article may be republished online under the CC-BY-NC-ND Creative Commons license.
The text must not be edited and the author(s) and source (Science Arena) must be credited.





