#News
#News
DATASUS: why Brazil collects so much health data—but still makes few decisions using it
Open-access databases have put Brazil on the global map, but fragmentation and gaps make it difficult to turn information into health decisions
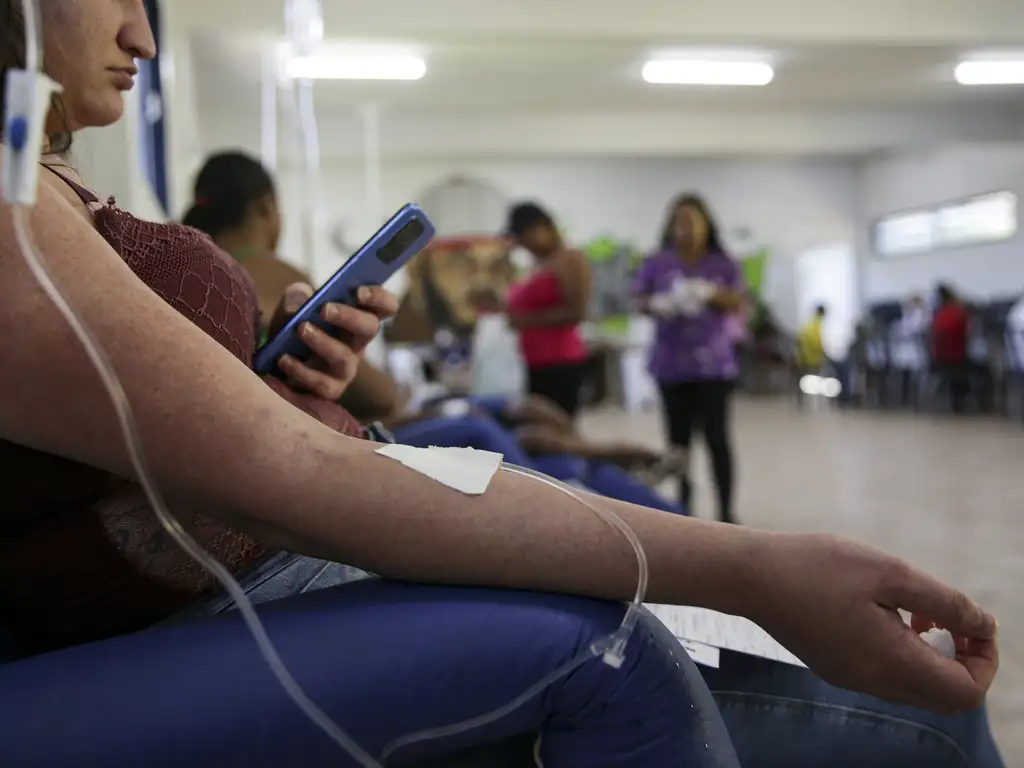
Brazil maintains one of the world’s most comprehensive public health data infrastructures: anyone can access information about mortality, births, hospitalizations, and disease notifications in the country without registration or authorization.
Compiled by DATASUS—the Department of Informatics of the Brazilian public health system (SUS), affiliated with the Ministry of Health—these databases support research that analyzes public policies and patterns of care within the SUS. Transforming all this information into sound management decisions, however, is still a challenge.
Created in 1991, DATASUS compiles and standardizes data submitted by states and municipalities. In its 34 years of operation, the department has developed over 440 information systems that directly support federal, state, and municipal public health system management.
In 2023 alone, the system recorded 13 million hospitalizations and 5.7 million surgeries—a snapshot of the scale of care delivery captured each month by DATASUS.
Death and live birth records exceed 95% coverage nationwide, enabling comparisons between regions.
“We can integrate all of this in the same system, regardless of whether the baby was born in the public or private system,” explains Alexandre Chiavegatto Filho, professor of Machine Learning in Health at the University of São Paulo (USP) and director of the Laboratory of Big Data and Predictive Analytics in Health (LABDAPS)
“Data from DATASUS are a global benchmark. In a country as vast and diverse as Brazil, the quality of our health data is impressive,” notes Chiavegatto Filho.
Hospitals, primary care units, outpatient services, and surveillance teams feed into databases such as the Hospital Information System (SIH/SUS), the Outpatient Information System (SIA/SUS), and the Notifiable Disease Information System (SINAN).
After consolidation and technical validation, the anonymized data are made available on open platforms such as TabNet. “Access is free, which is not the case in most countries,” says Chiavegatto.
From these databases, researchers build indicators, identify regional inequalities, and assess patterns of care. The analysis, however, encounters structural limitations in the system’s own design.
Although it records events—hospitalizations, procedures, and deaths—DATASUS does not automatically organize this information into clinical pathways. To turn numbers into evidence on care quality or spending efficiency, different databases need to be cross-referenced and data completeness gaps addressed.
Strategic data-use difficulties
One of the main obstacles is fragmentation between databases, which operate in parallel and follow different data entry rules. The gap was identified in a study by the Center for Studies and Promotion of Health Policies (CEPPS) at Einstein Hospital Israelita, published in Cadernos de Gestão Pública e Cidadania (Public Management and Citizenship Journals) in 2025.
When analyzing recorded surgical activity in the outpatient (SIA) and hospital (SIH) systems, the researchers encountered problems with completeness, trustworthiness, and specificity.
In 2023, 76.6% of outpatient surgeries were recorded without an ICD-10 code—the International Classification of Diseases, which identifies the diagnosis associated with each procedure.
In the hospital system, 10.6% of surgeries were recorded as multiple procedures, without itemized details. According to the authors, these inconsistencies hinder analyses of care delivery and management and limit the organization of the SUS into care networks.
“The databases do not communicate with each other. There is mandatory information in one system that is not required in another,” says Lucas Hernandes Corrêa, a researcher at CEPPS/Einstein.
This discrepancy prevents the linking of procedures to the condition that led to them. Even in the hospital system, where an ICD code is mandatory, some surgeries are recorded as multiple or sequential procedures, without sufficient detail to identify what was performed.
For SUS managers, researchers, and auditors, the practical effect is direct: “We have no idea which surgeries were performed on that patient. This makes it difficult to assess whether they were referrals or whether the payment is appropriate,” says Corrêa.
Further challenges
Another limitation is the inability to follow the care pathway of a single patient through the system. It is not possible to know, for example, whether a baby born underweight was hospitalized weeks later, or whether a pregnant woman who attended prenatal consultations experienced complications during labor.
Without this individual timeline, it is more difficult to establish relationships between risk factors, interventions, and clinical outcomes, and to apply predictive models. “The databases are independent from one another, which is a major limitation, including for the use of AI algorithms,” explains Chiavegatto.
“If we had this type of data, algorithms would be able to learn the characteristics associated with infant mortality and estimate risk probabilities, for example.”
Lack of formal channels hinders the incorporation of evidence into management
Even when data allow the identification of care delivery patterns, translating this evidence into management decisions is not automatic. At CEPPS, for example, an ongoing study is examining gallbladder removal surgeries (cholecystectomy), a highly prevalent procedure within the SUS.
Although there is well-established evidence that the laparoscopic technique is associated with better outcomes and shorter hospital stays, the data indicate that most are still performed using open surgery.
“DATASUS shows that we are still far from best practices in care delivery, which would be laparoscopic procedures. And this means we are not delivering the best possible outcomes for patients,” says Corrêa, from Einstein.
“We might be paying less for open surgery because it has a lower cost, but at the same time we are generating costs that we cannot necessarily see.”
The case illustrates another challenge: the lack of well-established institutional channels for incorporating research findings into management. Corrêa notes that there is still no structured methodology for systematically delivering this evidence to decision makers.
“What has been happening is that the doctors involved in these studies have taken these findings to medical societies and other institutions that discuss public policies in some way, but from a more technical and care delivery standpoint, not a management one,” he says.
Data guide decision-making In emergencies and structuring policies
Even so, there are situations in which using these databases has become central to administrative decisions. One example was the COVID-19 pandemic, when data on the daily progression of hospitalizations and deaths supported decisions on opening hospital beds, mobility restrictions, and resource allocation.
“The number of deaths and hospitalizations was a major motivator for COVID-19 control measures. From one week to the next, these data had a direct impact on the response to the pandemic,” states Chiavegatto, from USP.
Recent regulations have also strengthened the link between funding and care delivery reporting. In December 2025, Ministry of Health (GM/MS) Ordinance no. 9.037 made monitoring the allocation of parliamentary amendment funds for specialized care conditional on recording care delivery in systems such as SIA and SIH.
In practice, hospitals and services not adequately recording the procedures performed could compromise their funding allocations, making accurate database entry a direct condition for funding.
Well-established indicators, in turn, guide structural policies. According to Chiavegatto, the infant mortality rate is one of the most sensitive indicators in the field of health, because it tends to rapidly reflect disruptions in the system, such as the closure of maternity wards, sanitation failures, or food insecurity.
“All state health departments primarily use DATASUS data as a decision-making guide,” he says.
In a statement to Science Arena, the Ministry of Health stated that it has been adopting measures to improve and integrate national information systems, such as enhancing the Brazilian National Health Data Network (RNDS) and implementing the SUS Digital program, and that it considers scientific research and monitoring of SUS databases strategic for improving public policies.
The main DATASUS databases
1. SIM — Mortality Information System: records all death certifications in Brazil. Coverage exceeds 95% nationwide. Main source for calculating indicators such as the infant mortality rate.
2. SINASC — Live Birth Information System: records births, with data on pregnancy, childbirth, and newborn health. Coverage also above 95% nationwide.
3. SIH/SUS — Hospital Information System: records hospitalizations in public facilities and those affiliated with the SUS, collecting more than 50 variables per hospitalization—from diagnoses to procedures and length of stay. In 2023, just over 13 million hospitalizations were recorded.
4. SIA/SUS — Outpatient Information System: records procedures performed outside the hospital setting, such as outpatient consultations and surgeries. In operation since 1994.
5. SINAN — Notifiable Disease Information System: records notifiable diseases such as dengue, tuberculosis, and HIV.
6. TabNet: an open access platform that allows users to query all the databases above and tabulate data, without requiring registration or authorization.
*
This article may be republished online under the CC-BY-NC-ND Creative Commons license.
The text must not be edited and the author(s) and source (Science Arena) must be credited.